Trigeminal Neuralgia
This is a condition which may be treated by GP’s, Neurologists, Psychiatrists, Neurophysicians and Neurosurgeons. It is characterized by a severe spasmodic and lancinating pain which affects one side of the face.
The pain is excruciating, severe and is triggered by actions like chewing, swallowing, drinking hot or cold liquids, brushing the teeth, or being exposed to cold wind.
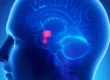
The cause of the symptoms is the pain which usually affects one branch of the trigeminal nerve which supplies sensation to the side of the face. In many cases symptoms seem to be related to a loop of a blood vessel within the brain itself pressing on the trigeminal nerve.
Prof. Shahzad Shams worked as Head and Professor of Neurosurgery Department at Lahore General Hospital, LGH, and presently works as Chairman Department of Neurosurgery King Edward Medical University and Mayo Hospital, Lahore, Pakistan
Treatment
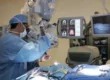
MVD Surgery
Endoscopic Microvascular Decompression
Endoscopic Microvasular decompression is a procedure in which a 2cm opening is made behind the ear and through this opening a endoscope of 4mm size is inserted to find the vessel. Which is offending oe pressing the trigeminal nerve which is then separated from the nerve using micosurgical instruments and a small Teflon graft is placed in between the vessel and nerve. Patient is immediately relieved of the severe pain on the face and is discharged within 24 hours from the hospital.
Results
The results for Endoscopic Microvascular decompression (MVD) are excellent and the procedure once done the patient is relieved of the pain forever and permanently. Hospital stay is only for 24 hours.